By Tara Mancini
Yesterday, three timely releases from the Kaiser Commission on Medicaid and the Uninsured show that state budgets are beginning to turn around. The 11th annual 50-state survey of Medicaid budgets, coupled with an updated brief on state budgets in recession and recovery, and another on Medicaid provisions in ARRA (the stimulus bill) show that the enrollment rate is slowing for a third year in a row and state revenues are rebounding for the sixth consecutive quarter. However, there will not be any jubilant celebrations emanating from states capitals just yet as this fiscal year states are facing an increasing share of Medicaid costs.
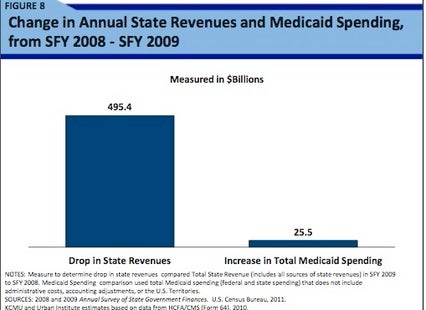
Say Ahhh! readers are acutely aware that the reason for this increase in states’ shares of spending is the June 2011 expiration of the enhanced matching rate in ARRA. According to the updated Kaiser brief on state budgets in recession and recovery, the federal government spent almost 90 billion dollars in state fiscal relief by increasing its share of Medicaid FMAP funds. While total Medicaid spending only increased by 7.6% in FY2009, enhanced FMAP funds were especially vital given the 30 precent drop in state revenues. These federal funds helped to cover the increases in enrollment as many found themselves out a job and losing their employer-based coverage.
Even with Medicaid enrollment slowing, the loss of federal stimulus dollars has left states feeling strained when it comes to paying for Medicaid. According to the budget survey, total Medicaid spending in fiscal year 2012 is projected to grow at a rate of only 2.2%, making it the second slowest growth rate in the last 12 years. Yet states are expected to see a 29% increase in spending as a result of the lost federal funding.
In coping with this increased responsibility, states have set out to try to contain costs; for example, a majority of states adopted provider rate restrictions, while some have also instituted benefit reductions and restrictions and newer and higher co-payments for beneficiaries.
However, it is important to note that despite the trying circumstances, states are also looking to deliver better care and prepare for health reform. In fact, the report finds that 37 states have submitted letters of intent to work with CMS on more effectively coordinating care for dual eligible populations. States are also continuing to shift the delivery of long-term care to the community and away from institutions.
Additionally, a number of states are expanding Medicaid managed care (24 states in 2012). It’s not always clear about what the motivations are behind the changes – some may be interested in improving care management and coordination, others may wish to gain more predictability in spending or increase accountability for access to providers and quality of care.
Even though states made some budget cuts in Medicaid, overall, the report finds that the stability protections in both ARRA and health reform prevented states from restricting their Medicaid eligibility standards, and despite their dire budgets, many states reported eligibility expansions or enrollment simplifications. As evident by the impact that the increased ARRA funding had on states’ ability to respond to the economic crisis and growing enrollment, states need a stronger commitment from their federal partner in the program, not more cost-shifting to states.