All
-
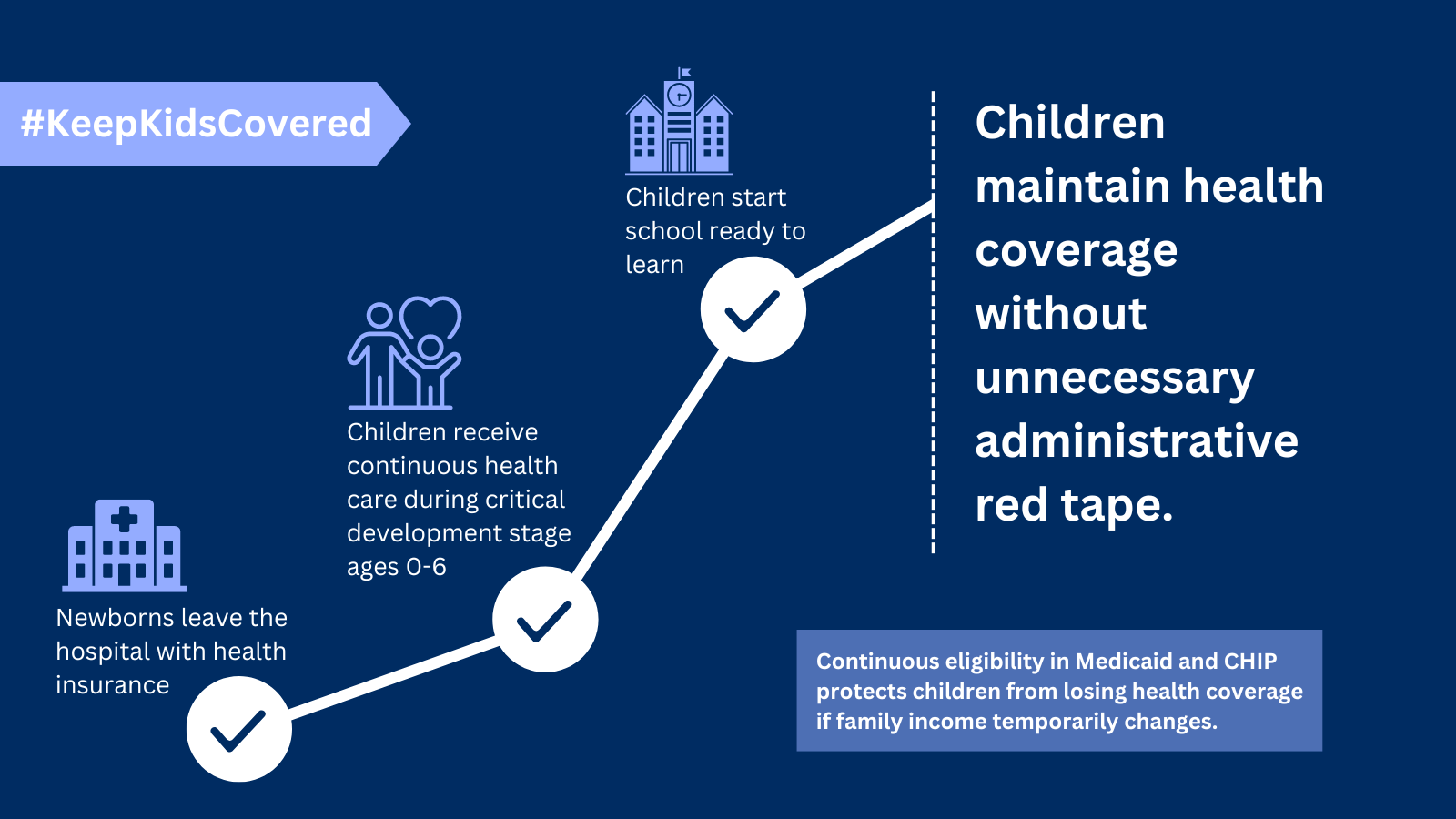
Multi-Year Continuous Eligibility for Children
As of January 1, 2024, all states are required to provide 12 months of continuous health coverage for children in Medicaid and the Children’s Health Insurance Program (CHIP). This reduces the risk of eligible children losing coverage due to administrative barriers or temporary fluctuations in family income. In 2022, Oregon became the first state approved…
-
Research Shows Medicaid Expansion Beneficial to Child Health and Family Financial Security
While the Affordable Care Act’s Medicaid expansion was designed to help the large number of uninsured adults who could not afford private insurance, the policy change has proven to be immensely helpful to children too. In February 2021, we released a report on the critical link between Medicaid expansion for adults and improvements to child…
-
It’s Unanimous: CMS Needs to Bring More Transparency to Medicaid Managed Care
Last week, MACPAC Commissioners voted to recommend that the Centers for Medicare & Medicaid Services post all state Managed Care Program Annual Reports (MCPARs) to the CMS website. The vote was unanimous: 17-0. The recommendation will be included in MACPAC’s March 2024 Report to Congress. At first glance, this may seem unremarkable, but on further…
-
CCF Comments on Questions from the Task Force on Maternal Mental Health
The Georgetown University Center for Children and Families submitted the following comments to the Office on Women’s Health at the U.S. Department of Health and Human Services regarding questions from the task force on maternal mental health. Read the Comments
-
CCF Comments on the Interim Final Rule on CMS Compliance with Reporting and Federal Medicaid Renewal Requirements
The Georgetown University Center for Children and Families submitted the following comments to the Centers for Medicare & Medicaid Services regarding the interim final rule on CMS enforcement of state compliance with reporting and federal Medicaid renewal requirements under Section 1902(tt) of the Social Security Act (CMS- 2447). Read the Comments
-
Momentum for Community Health Workers in Medicaid Continues in the New Year
For some good news to start 2024, the gains for community health workers (CHWs) in the Medicaid world continue to increase. We’ve written about the value of Medicaid as a sustainable funding source for CHW services and growing efforts in states previously here on Say Ahhh!…but wait, there’s more! Michigan has integrated CHWs in targeted…
-
Most States Show Improvement in Automated (Ex Parte) Medicaid Renewal Rates
Although ex parte was hardly a household term before the unwinding of the Medicaid continuous enrollment requirement, most stakeholders and observers are now aware of the critical role automating renewals using data available to the state can play in reducing churn and promoting continuity of coverage in Medicaid and CHIP. The policy not only removes…
-
How many people are applying or reapplying for Medicaid?
Medicaid and CHIP Monthly Application Volume The charts below show trends in each state’s monthly application volume during the unwinding. This analysis is based on monthly application data reported to CMS by state Medicaid and CHIP agencies. Application volume captures the number of applications submitted and is not a count of individuals seeking coverage. It…
-
CMS Announces $50 Million in Capacity Building Grants for Medicaid/CHIP School-Based Health Services
This week, the Centers for Medicare & Medicaid Services (CMS) announced a Notice of Funding Opportunity for the much anticipated planning grants to implement or expand school-based health services for children enrolled in Medicaid and CHIP. As we’ve written about in previous blogs, the Bipartisan Safer Communities Act appropriated $50 million in grants for states…
-
New Report Outlines Opportunities for States to Leverage Medicaid to Improve Mental Health of Postpartum Moms and Babies
By: Anne Dwyer, Elisabeth Burak, Tanesha Mondestin, and Kay Johnson As we recognize Maternal Health Awareness Day, it’s a good time to take stock of where the U.S. stands in advancing maternal and child health. The relatively new state option to extend Medicaid postpartum coverage from 60 days to one full year provides states with…
-
State Medicaid Opportunities to Support Mental Health of Mothers and Babies During the 12-Month Postpartum Period
Download Full Report (PDF) By: Elisabeth Burak, Anne Dwyer, Tanesha Mondestin, and Kay Johnson Most states have moved to adopt a new state option to extend Medicaid coverage to all enrolled pregnant people from 60 days to 12 months following a pregnancy. As the predominant payor of U.S. births and health care to postpartum people…
-
CMS Announces New State Opportunity to Advance Behavioral Health Care Integration
Last week, the Centers for Medicare & Medicaid Services (CMS) announced a new state opportunity to test approaches for addressing behavioral, physical, and health-related social needs of individuals covered by Medicaid and Medicare. Structured as a new “Innovation in Behavioral Health” (IBH) model to be tested by the CMS Innovation Center, the state-based model is…
-
CMS Unsurprisingly Concludes Georgia Demonstration Extension Request Is… An Extension Request
On December 22, CMS sent Georgia a letter confirming that the state’s section 1115 demonstration extension request was being reviewed as an extension request. This straightforward conclusion, which the state was trying to avoid, has some important consequences for the state’s on-going Medicaid expansion debacle. But let’s start with the background. In February 2023, Georgia…
-
CMS Previews State Grants to Transform Maternal Health, Grow Community-Based Workforce
Many states have been taking a closer look at the experiences of pregnant and postpartum people amidst the persistent maternal health crisis, including reaching communities– most especially Black and Indigenous women and other communities of color who have not fared well in the traditional, clinical health care system. We at CCF have championed states electing…
-
Federal Poverty Levels Rise 4.1 Percent on Average
HHS has released the 2024 federal poverty levels (FPLs) that will be used for means-tested public benefits, including Medicaid and CHIP. This means the annual poverty level for a family of three has increased to $25,820 up from $24,860 in 2023. The poverty level for an individual has increased from $14,580 to $15,060. It’s important…
-
Latest Data Show Marketplace Enrollment Rate Up Slightly Among Those Losing Medicaid Coverage During Unwinding
As readers of Say Ahhh! know, I have been tracking monthly data (here, here, here, here and here) from the Centers for Medicare and Medicaid Services (CMS) on the number of people who were either previously enrolled in Medicaid or had experienced a denial or termination who then selected a marketplace plan. At the end…
-
Child Medicaid Enrollment Decline Reaches 3 Million: How Many Kids are Moving to CHIP?
Our tracker of net child Medicaid enrollment declines during the unwinding period just reached, and then quickly exceeded, 3 million with the release of October data by Texas – the undisputed national leader in dumping kids off Medicaid. In February 2022, Georgetown CCF researchers projected that as many as 6.7 million children could experience a…
-
Program Assistant
The program assistant will provide research and administrative support to CCF, primarily but not exclusively to the Center’s maternal and early childhood team. This position requires a high level of competence and commitment, interest in health policy that addresses health equity, as well as a wide range of administrative, communications, and administrative management skills. The…
-
Zero to Six Continuous Coverage Proposed in Pennsylvania, Approved in New Mexico
As we hit the milestone of 3 million children losing Medicaid coverage in less than a year, movement toward multi-year eligibility in Medicaid continues to be a bright spot in the unwinding storm. Last week CMS approved New Mexico’s request to implement continuous coverage for children up to age 6, joining Oregon and Washington in…
-
As Extra Medicaid Funding Phases Out at Year’s End, States Must Still Report Data and Comply with Federal Renewal Requirements
Starting in 2024, states will no longer receive extra federal funding associated with the Medicaid continuous enrollment requirement that was in place from March 2020 through March 2023. But the recent Interim Final Rule with Comment (IFC) released by CMS reminds states that they must continue to meet data reporting requirements specified by Congress and…