The September 30 expiration of federal CHIP funding puts the New York program, Child Health Plus (CHP) in a precarious situation. Data from the new UHF HealthWatch brief, The Curve Bends Back Up, Sharply, suggests that CHP is growing in its importance – which means insurance coverage is at risk for more New York children than we expected if federal funding is not reauthorized soon.
For over thirty years, throughout changes in political party leadership and the state’s economic health, New York State has used state funds to assist lower-income families to afford health insurance coverage for their children. The passage of the federal Children’s Health Insurance Program in 1997 made it possible for the Child Health Plus program to closely mirror the state Medicaid child benefit package, except for long term care. Almost all the health plans participating in the state’s Medicaid program also offer a CHP product, and the state requires them to use and report on the same quality measures. As noted in a UHF report last March, their scores reflect generally high quality care, often exceeding national averages for Medicaid plans.
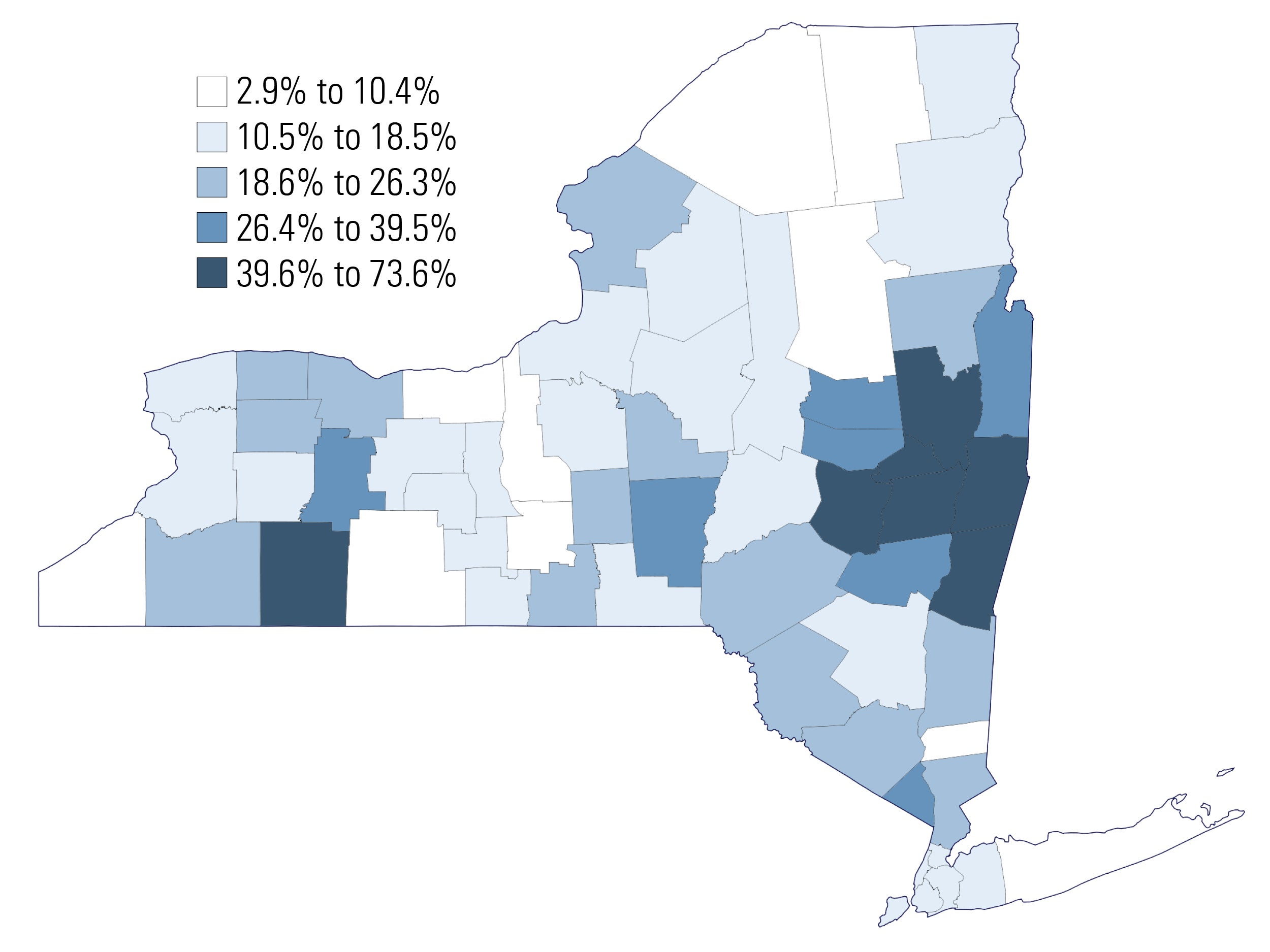
As Tricia Brooks noted last week, the number of states that expect to exhaust their federal CHIP funding before the end of 2017 has now jumped from four to ten. New York State is not one of those ten, but is coming very close. Enrollment in CHP has soared by an unexpected 17 percent since July of 2016, to a monthly enrollment figure of 347, 855 in July 2017 and 350,195 as of September. Most of the growth occurred outside New York City, with the largest percentage increases occurring in the greater Albany area and the southwestern part of the state. While it is not clear what precipitated this marked jump in enrollment, one factor may be the aggressive outreach effort launched across the state in early 2016, when the state implemented its new Basic Health Program, the Essential Plan, for adults with a family income below 200 percent of poverty. Although children are not eligible for coverage under the Essential Plan, the outreach effort may have found families unaware of the availability of CHP. We do know that approximately 40 percent of the enrollees are from families with incomes between 150 percent and 200 percent FPL.
While the Oct. 4 approval of legislation extending federal CHIP dollars for five more years by both the Senate Finance Committee and the House Energy and Commerce was welcome news to our child health community, serious objections to the offsets identified by the House committee to fund the extension threatens further progress. We hope the Congress will move swiftly to resolve those problems and end the uncertainty for New York’s 350,000 children and their families.
[Lee Partridge serves as an advisor to the Children’s Health Initiative, United Hospital Fund and Misha Sharp is a research analyst in the Medicaid Institute, United Hospital Fund. The United Hospital Fund is an independent, nonprofit organization working to build a more effective health care system for every New Yorker. For more information, visit www.uhfnyc.org.]