All
-
Limited Child Medicaid Unwinding Data Begins to Paint Bleak Picture, Highlights Need for More Transparency
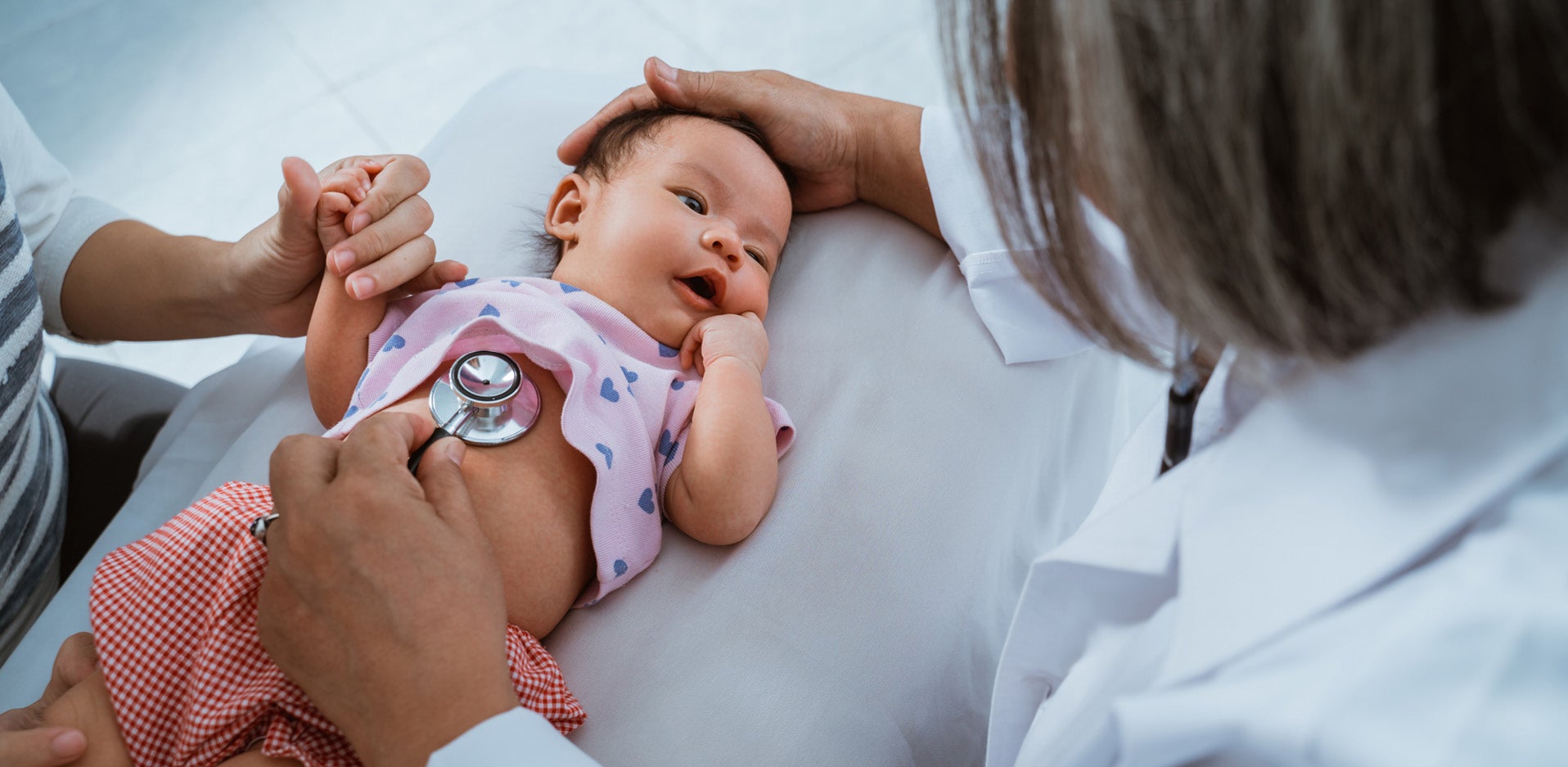
As we continue to unpack the first round of unwinding data released by CMS a few weeks ago, it remains disappointing that there is not more data on children. As readers of SayAhhh! know, the stakes for children are very high with over half of the children in the country insured through Medicaid, and they…
-
Medicaid Managed Care: Early Results of the PHE Unwinding for the Big Five in Q2 2023
The Medicaid enrollment results for the “Big Five” during the quarter ending June 30 are now in. The Big Five have the largest share of the Medicaid managed care market: Centene, CVSHealth (Aetna), Elevance Health (formerly Anthem), Molina Healthcare, and UnitedHealth Group. They, along with two large nonprofit companies, were the focus of a recent…
-
Understanding the Medicaid Unwinding Data: Marketplace Enrollment
On July 28, 2023, the Centers for Medicare and Medicaid Services (CMS) finally released renewal outcome data from the first two months — March and April 2023 — of unwinding of the Medicaid continuous coverage protection. The data is largely consistent with data that we have already posted in our tracking of state administrative unwinding…
-
Data shows kids greatly impacted by KanCare redeterminations
By Heather Braum, Kansas Action for Children Kansas released the second set of data for how the year-long KanCare unwinding process is going, with data available through June 30, 2023, and has now broken out the data into age ranges and by county for those who had not returned a renewal form in April or May. Since…
-
First Batch of CMS Unwinding Data Includes Key Call Center Statistics
Last Friday, CMS released the first round of long-anticipated Medicaid unwinding data. The main focus has been on the renewal outcome data submitted in state monthly reports, which unfortunately was only available for the 18 states who began terminating coverage as of March 31 or in April 2023 due to a lengthy lag – and…
-
Medicaid Managed Care: Denials of Prior Authorization for Services
Kudos to the OIG! That would be the Office of the Inspector General of the Department of Health and Human Services. Although OIG is better known for its fraud-fighting persona, it also has a broader mission of making government programs work better. And with last month’s report, “High Rates of Prior Authorization Denials by Some…
-
Administration Releases Medicaid and CHIP Mental Health and SUD Action Plan, Parity Initiatives
In another round of mental health-related announcements, this week, the Centers for Medicare & Medicaid Services (CMS) released a Medicaid and CHIP Mental Health and Substance Use Disorder Action Plan alongside Administration announcements focused on mental health parity. The seventeen page Mental Health and Substance Use Disorder Action Plan provides an overview of Medicaid and…
-
Transparency, Trackers, and Toolkits: Updates on CCF Unwinding Materials
By Ella Mathews and Shreya Kalra As Unwinding Wednesday readers know, our 50 State Unwinding Tracker is updated regularly as we monitor new information, specifically new unwinding data, provided by states. The tracker has evolved since we released it almost a year ago – both in the number of states publicly providing unwinding information and…
-
Legislative Roundup: Eight states now committed to multi-year continuous eligibility for young children as Colorado, Minnesota and Ohio pass new legislation
The unwinding continues to dramatically showcase children’s loss of health care despite the fact that most likely remain eligible. Amid the worse-than-expected disenrollments among children due to red tape and insufficient communication, one bright spot is that more states are seeking CMS approval to reduce administrative burden on families by adopting 2-to-5 year continuous eligibility…
-
-
The Medicaid Unwind’s Impact on Children: Are They Moving to CHIP?
As of July 1st all states in the country (except for Oregon) have started the process of renewing and disenrolling children and adults from Medicaid according to CMS’s latest chart. As readers of SayAhhh! are well aware, states are checking eligibility for everyone enrolled in Medicaid after the continuous coverage protections associated with the COVID-19…
-
Protected: CCF Annual Child Health Policy Conference 2023
There is no excerpt because this is a protected post.
-
What is happening with Medicaid renewals in each state?
The analysis on this page is part of a larger suite of Medicaid unwinding data. Please visit our “Unwinding the PHE” landing page to view more. This interactive chart shows outcomes of Medicaid renewals since the lifting of the COVID related continuous enrollment requirement on March 31, 2023, making April the first month in which…
-
Expanding Options to Identify Renewal Dates Could Help Minimize Procedural Disenrollments
We’re only four months into the Medicaid unwinding and the scale of coverage loss for procedural reasons is already staggering. An estimated 1.6 million individuals have lost coverage, with 71 percent terminated for procedural reasons. Stories are trickling in about why these procedural disenrollments may be occurring, including families not getting notices in the mail.…
-
CCF Comments on Proposed Managed Care Rule
The Georgetown University Center for Children and Families submitted the following comments to HHS regarding the proposed managed care rule (“Medicaid Program; Medicaid and Children’s Health Insurance Program (CHIP) Managed Care Access, Finance, and Quality; Proposed Rule-CMS-2439-P”). Comments on Managed Care Rule
-
CCF Comments on Proposed Access Rule (CMS-2442-P – “Medicaid Program; Ensuring Access to Medicaid Services”)
The Georgetown University Center for Children and Families submitted the following comments to HHS regarding the proposed access rule (“Medicaid Program; Ensuring Access to Medicaid Services – CMS-2442-P”). Comments on Proposed Access Rule
-
Georgetown CCF Analysis Finds Georgia’s Pathways to Coverage Program Would Cost More to Cover Fewer People
This week, we released a new analysis, written by Allexa Gardner, Joan Alker and Leo Cuello, that finds Georgia’s limited Medicaid expansion program, known as “Pathways,” is fiscally foolish and sets up a structure that discriminates against parents. Enrollment for Pathways begins on July 1st with coverage being at a later date likely September 1.…
-
Research Update: This Pride Month, We Celebrate Improvements in Coverage and Access for LGBTQ+ Adults
This week I am proud to highlight two recent studies showing that adults identifying as lesbian, gay, bisexual, and transgender (LGBT) have made significant gains in coverage and access to care over the past several years since the Affordable Care Act (ACA) and its Medicaid expansions have taken effect. LGBT adults have historically faced serious…
-
An Analysis of Georgia’s Section 1115 Medicaid Pathways to Coverage Program
Download Full Report In July 2023, Georgia will begin enrollment into its new Medicaid Pathways to Coverage (“Pathways”) program, with coverage expected to begin in September 2023. The program would offer coverage to a subset of low-income adults who meet a work reporting requirement and, depending on their income, pay a monthly premium. Georgia will…
-
Comments on Utah Medicaid Reform 1115 Demonstration Amendment Request for Postpartum Coverage Extension
The Georgetown University Center for Children and Families in conjunction with the Center on Budget and Policy Priorities submitted the following comments to HHS regarding the proposed postpartum coverage extension in Utah. Utah Postpartum Coverage Extension Comments